Know Your Risk. Protect Your Health. Save Lives.
Anal cancer is one of the most preventable forms of cancer—yet it remains underdiagnosed and often overlooked in routine care. For many individuals, especially those in higher-risk communities, a simple screening test can make the difference between early treatment and advanced disease. Despite this, awareness around anal cancer screening remains low. Stigma, lack of provider education, and limited access to specialized care all contribute to missed opportunities for prevention.
At Inclusive Care Group, we believe that prevention starts with education—and that everyone deserves access to proactive, stigma-free healthcare.
Understanding Anal Cancer
Anal cancer develops in the tissues of the anal canal and is most commonly linked to persistent infection with Human Papillomavirus (HPV). This is the same virus responsible for nearly all cases of cervical cancer, as well as many throat and genital cancers.
In most people, HPV clears naturally. However, in some individuals—particularly those with weakened immune systems—the virus can persist and cause abnormal cellular changes over time.
These changes can progress from:
- Normal cells
→ Low-grade lesions
→ High-grade squamous intraepithelial lesions (HSIL)
→ Anal cancer
The key takeaway: anal cancer does not develop overnight. It often takes years, which makes early detection both possible and highly effective.
Why Anal Cancer Screening Matters
Anal cancer is still considered rare in the general population, but incidence rates are rising—especially among high-risk groups.
Research shows:
- Individuals living with HIV are 15 to 20 times more likely to develop anal cancer compared to the general population
- Men who have sex with men (MSM) have significantly higher rates of HPV-related anal disease
- Persistent HPV infection is the primary driver of anal cancer
One of the most important breakthroughs in prevention comes from the landmark ANCHOR study, led by the National Institutes of Health and published in the New England Journal of Medicine.
The study found that:
Treating high-grade precancerous lesions (HSIL) reduced the risk of developing anal cancer by approximately 57%.
This confirms what many clinicians have long believed: screening and early treatment save lives.
What Is Anal Cancer Screening?
Anal cancer screening is designed to detect abnormal cells before they turn into cancer.
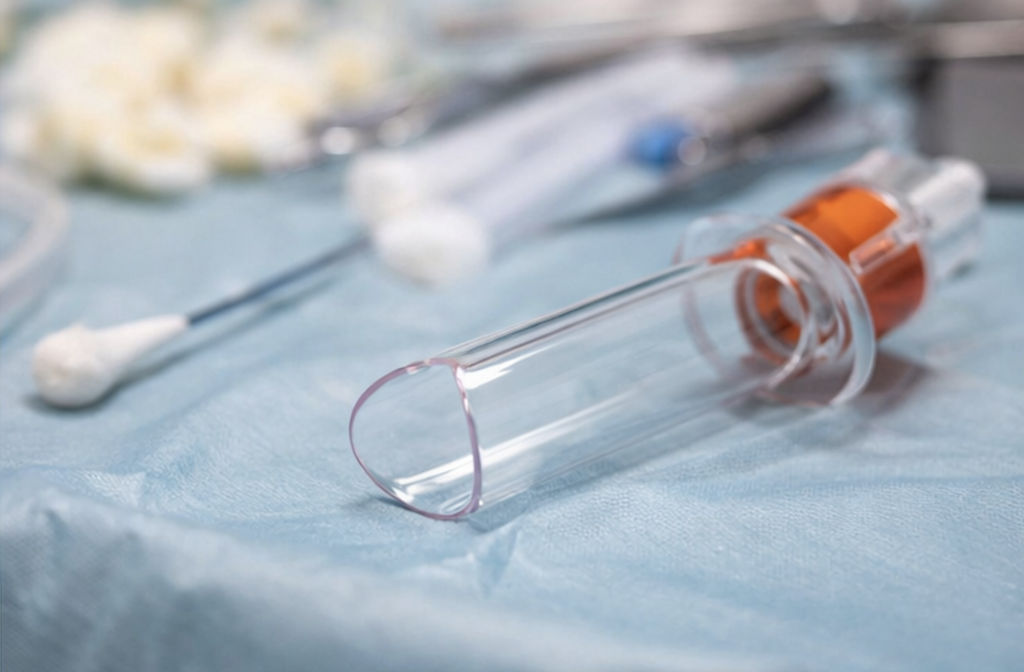
The most common method is the anal Pap test (anal cytology), which works similarly to a cervical Pap smear:
- A soft swab is used to collect cells from the anal canal
- The sample is sent to a lab to check for abnormal or precancerous cells
- The procedure is quick, minimally invasive, and typically takes less than a minute
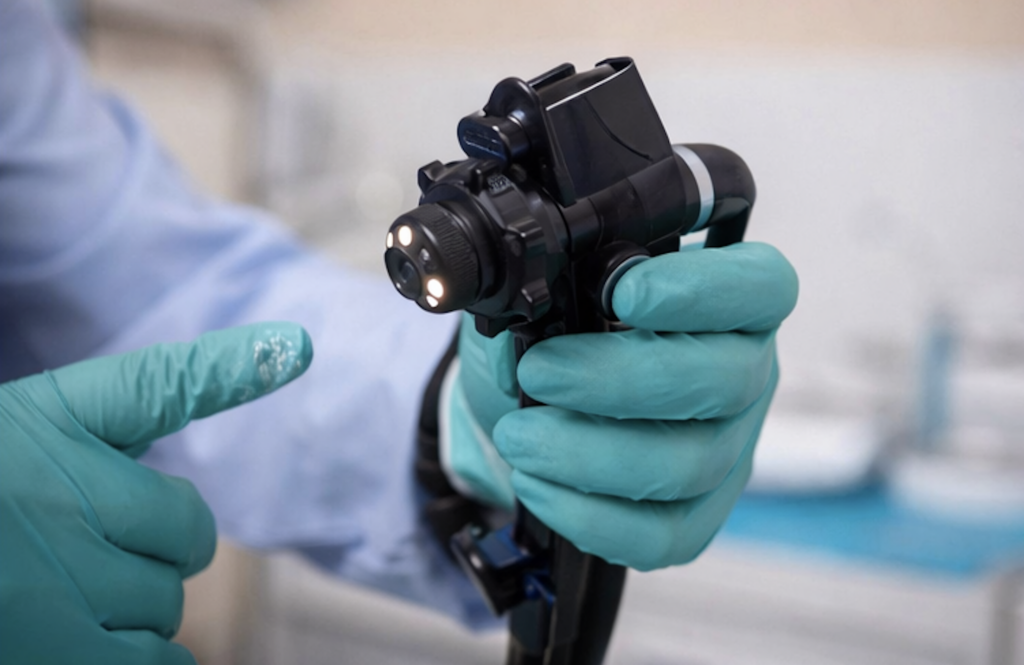
If abnormalities are detected, patients may be referred for high-resolution anoscopy (HRA)—a specialized procedure that allows providers to closely examine and biopsy suspicious areas.
Who Should Be Screened?
Screening is especially important for individuals at increased risk.
People Living with HIV
- MSM and transgender women: Start screening at age 35
- All other individuals with HIV: Start screening at age 45
Other High-Risk Groups
- Solid organ transplant recipients (start 10 years post-transplant)
- Individuals with a history of:
- Cervical, vaginal, or vulvar cancer or precancer
- Persistent HPV infection
- Genital warts
- MSM without HIV: Consider screening starting at age 45
- Anyone who has receptive anal intercourse
Guidance from organizations like the Infectious Diseases Society of America and HIV Medicine Association supports integrating anal cancer screening into
What Happens After Screening?
Understanding the process helps reduce anxiety and increases follow-through.
1. Normal Results
Continue routine screening (typically annually for high-risk individuals)
2. Abnormal Results
Referral for high-resolution anoscopy (HRA)
3. If Precancer (HSIL) Is Found
Treatment options may include:
- Electrocautery (heat-based removal)
- Topical therapies
- Minor surgical procedures
4. Ongoing Monitoring
Regular follow-up is essential to prevent progression or recurrence

Breaking the Stigma Around Screening
One of the biggest barriers to anal cancer screening isn’t access—it’s discomfort.
Many patients avoid screening due to:
- Embarrassment
- Fear of judgment
- Lack of open conversation around sexual health
This is exactly why inclusive, affirming healthcare matters.
At Inclusive Care Group, we center care around dignity, respect, and trust. Conversations about sexual health, HPV, and screening are normal, medical, and necessary.
You deserve care that sees you—not just your chart.
Prevention Beyond Screening
Screening is powerful—but it’s just one part of prevention.
Additional strategies include:
- HPV vaccination (recommended up to age 45 in many cases)
- Routine STI screening
- HIV prevention and treatment (including PrEP and viral suppression)
- Smoking cessation, which reduces cancer risk
The Centers for Disease Control and Prevention emphasizes that combining vaccination, screening, and early treatment is the most effective way to reduce HPV-related cancers.
Take Action Today
Prevention starts with a conversation.
If you are at increased risk—or unsure if you are—talk to your healthcare provider about anal cancer screening.
At Inclusive Care Group, we’re here to provide comprehensive, judgment-free care that meets you where you are.
Because early detection doesn’t just improve outcomes—it saves lives.
If you have any questions or would like to schedule an appointment, feel free to call us at (727) 753-7787 or message us by clicking the link below.
References
- Centers for Disease Control and Prevention. Anal Cancer and HPV.
https://www.cdc.gov/cancer/anal/ - National Cancer Institute. Anal Cancer Prevention (PDQ®).
https://www.cancer.gov/types/anal - National Institutes of Health. ANCHOR Study Findings (2022).
- New England Journal of Medicine.
Palefsky JM et al. Treatment of Anal High-Grade Squamous Intraepithelial Lesions to Prevent Anal Cancer (2022) - Infectious Diseases Society of America & HIV Medicine Association.
Primary Care Guidelines for Persons with HIV - American Society for Colposcopy and Cervical Pathology.
Practice Advisory on Anal Cancer Screening
- Centers for Disease Control and Prevention. Anal Cancer and HPV.

